|
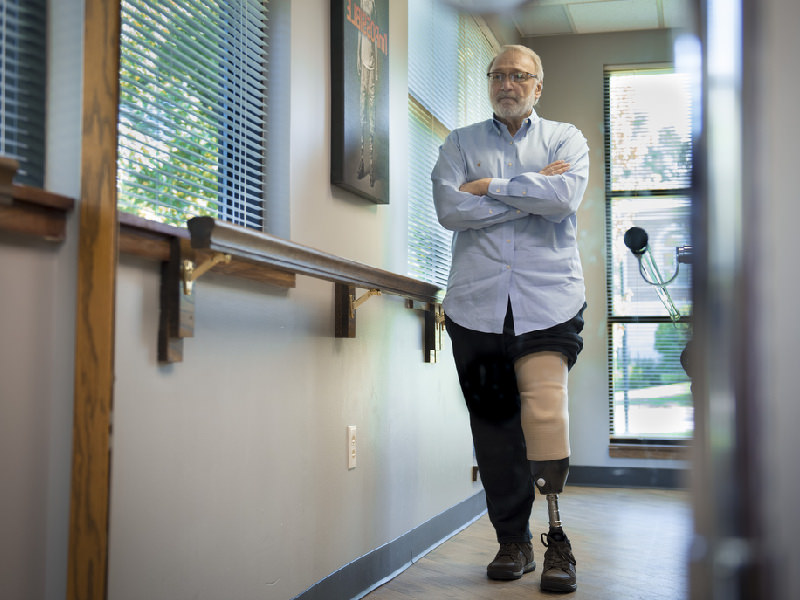
By Muniyra Douglas Transcribed by Tashia Antoine An amputation is a life changing event that requires approaching life in a whole new way. It is therefore necessary to encourage the promotion of inclusion and accessibility in our communities, work environment and society for Canadians of all abilities. A change in perspective about accessibility is being brought to light through a program in the Greater Toronto Area (GTA) that is helping amputees to recover and achieve their full potential. The West Park Healthcare Centre is the largest in-patient amputee service in Canada and is dedicated to assisting the amputee population with services that include physical, psychological and social benefits. In this VIBE TALKS interview Correspondent Muniyra Douglas speaks with Dr. Michael Devlin – Specialist, Amputee Rehabilitation at the West Park Healthcare Centre about the centre’s amputation recovery program - which is the only one in the GTA. We also discuss the program requirements, government assistance and some of the challenges and misconceptions patients may face while considering or during rehab. Muniyra: What are some of the focus areas for the Amputee Rehabilitation Program? Dr. Michael: We have both an inpatient and an outpatient program. The inpatient program has twenty one beds. These are basically individuals who by and large have just had a recent amputation, and are having their initial rehabilitation. The outpatient side, could again be people who have had a recent amputation, but don’t need to be in the hospital and can commute back and forth for outpatient therapy or outpatient follow up clinics. We follow these people basically for life after they’ve received their artificial leg or arm. Muniyra: What are some of the program requirements? Dr. Michael: You have to be over 18 years old. As far as fitting with the prosthesis, number one the patient must want to have the prosthesis. Number two, the rehab team here has to feel that they would benefit from and would use a prosthesis. It’s not common, but there are particularly, elderly people who have had an amputation above the knee and a prosthesis at that level is a fair amount of work, so they may really feel it’s not worth their while. Muniyra: How are costs typically covered? Dr. Michael: In Ontario, there is this thing called the Assistive Devices Program from the Ministry of Health and Long Term Care. It pays for 75% of the cost of the basic components for the artificial legs. If you put parts into it that are not basic, that are kind of moving up market, they don’t pay anything extra for that. They just pay for the basic components, so it becomes due on the patient to find the extra money, or their insurance company, or family, or what have you. Muniyra: What are some common misconceptions surrounding artificial limb recovery? Dr. Michael: There is a lot of press, I guess, about the high end components that are now available. Some patients think that this will be “the end all and be all” that is going to make them great. That is just not true. So I think the expectations on patients of what the high-end technology will actually do for them, are in excess of what it will do for them. Because these are expensive pieces. If you walk relatively poorly, as an above-knee amputee, fitting an expensive knee joint into you isn’t actually going to make you walk any better. Muniyra: For the prosthetic service, what are some challenges that might come with product fitting? Dr. Michael: The keystone to the whole thing is actually the socket, the part that the residual limb fits into. If it fits well, is comfortable, and is tolerated, then you are off to a great start! It does happen from time to time that patients just don't like the feel or the fit of the sockets or run into problems of skin breakdown, or complain about the weight. That is more an issue earlier on, because initially after you have an amputation, the residual limb will swell and when you fit them with an artificial leg, it will then shrink. There are a lot of changes and modifications that have to be done to the socket as the individual starts using their prosthesis. They keep on shrinking, and you have to keep chasing the shape of the residual limb. That can require a fair number of visits to see through the process and have those adjustments made. So, the first nine to twelve months, tends to be a pretty fluid situation. Muniyra: How might amputation affect a patient’s social or psychological state? Dr. Michael: The psychological issue may or may not play a role. Your typical amputee has the complication of diabetes. That’s the big one in our society. These are individuals who had skin sores or foot infections, ongoing from weeks to months to years, and they eventually come to an amputation. If you elect to step it forward for them, they are now free from being trapped at home having home care coming to do dressing changes all the time, or going to clinics all the time. It is kind of a finite end to the way they were, and it’s a new beginning. That population tends not to have much psychological issues relating to it. Whereas, individuals having an acute amputation, with a workplace injury or motor vehicle accident; they often do have much more psychological issues related to amputation, like post-traumatic stress disorder and stuff like that. Those things can actually be their biggest problem, and not the amputation. So, we do have in-house psychology, who can see these individuals. But we are a little limited over the long-term, so if someone does needs long-term mental health care, then we refer them to a community based psychologist or psychiatrist. Typically, it would be a psychiatrist because most of these patients, they can’t afford to pay for psychology, whereas psychiatry is covered under OHIP. Muniyra: Looking back to the last 10 or 15 years, how have tech advancements contributed to a more accessible lifestyle? Dr. Michael: In the last 10 to 15 years, I guess the changes that have been coming about over that timeframe is newer methods of suspensions; newer methods of holding the prosthesis onto the residual limb, which work better than our older ones. And, if they work better, the prosthesis feels lighter, you have less skin issues, less paraphernalia and you can get rid of a lot of belts and stuff like that, and that is one advantage. Advantage number two, is the materials of some of the socket liners has been advancing over the last 20 years or so. So, if you've got someone who has got scarring, a previous burn, or just kind of skin on bone these new liners allow for much better tolerability of the socket, than what we had previously. There has been an explosion in artificial knee technology for prostheses. So we’ve got computerized Microchip controlled knees which don’t buckle if you are going down a hill or trip over a curb. They also allow you to walk with variable speeds, which the older ones tend not to. The problem is that they are really pricey. Typically, the only people who can afford them are people who have got third party coverage elsewhere such as Worker’s Compensation or Auto Insurance. Muniyra: Does the Centre work with other related organizations within the industry? Dr. Michael: Yes, and No. Yes, we are doing research. Our research is primarily geared so far to looking at number one; outcome measures, because historically there have been very few, if any, outcome measures for amputee rehabilitation. It would be nice to show that what you are doing is actually worthwhile. So that is one area of work that we’ve now got some outcome measures for. Number two is research that has been looking at the number of falls because these people do fall a lot. We have looked a little bit at componentry in comparing one type of the same knee unit to another type of knee unit. But we are not doing research with the manufacturers. For example, if they come up with a new foot, we are not doing research or evaluating whether that foot is good, bad or indifferent. Muniyra: What are some suggestions that you have for patients in order to gain their confidence and to help them live an active lifestyle? Dr. Michael: Basically, you can encourage them to be as active as possible. A lot of these people have got a lot of other issues going on. With diabetes, impaired vision, impaired kidney function, impaired heart function, the amputation is just one of the things. In the younger population, which are primarily well other than their amputation, again we encourage them to be active. We’ve got contacts with amputee sporting organizations. A number of our younger patients do participate, and there is a lot of informal peer support out there amongst the amputees as far as that is concerned leading to amputee volleyball, and a number of other sporting activities. A lot of that is actually done in the community through peer contact between different amputees. These guys and girls come in to see their process and will see someone else similar in age, a younger person typically, and they will chat and one will say: “I’ve been doing this” and the other would say: “Whoa, this is kind of neat.” I think it is a situation where it works better with peer to peer interaction, rather than an organization or institution.
|
Recent Posts
Categories
All
Archives
February 2022
|
|
GET THE APP!
Listen to VIBE 105 anywhere you go!
|
OUR STATION
|
TUNE IN RADIO
|
STAY CONNECTED
|
Copyright © 2021 Canadian Centre for Civic Media and Arts Development Inc. Except where otherwise noted, presentation of content on this site is protected by copyright law and redistribution without consent or written permission of the sponsor is strictly prohibited.








 RSS Feed
RSS Feed


