|
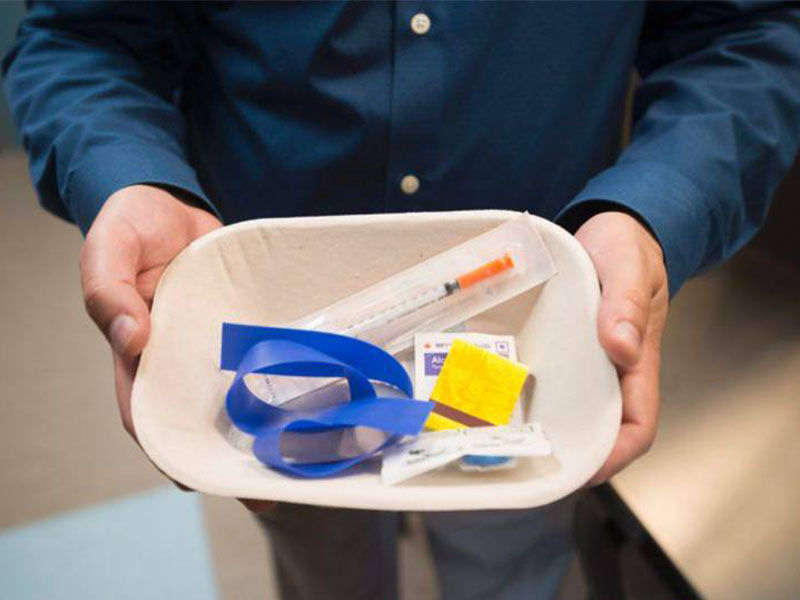
By Nina Kalirai Imagine a place that operates as a safe space for users to inject pre-obtained drugs, while under the supervision of a trained nurse. Well, think no more, as Toronto recently witnessed the opening of the permanent safe injection site: The Works, located at 277 Victoria Street. Being the first of its kind in the city, it has prompted many questions from the public regarding the exercise of safe drug usage on these sites. In the following interview by VIBE TALKS correspondent Nina Kalirai, we explore how exactly these safe-injection sites operate. We also discuss other services offered at The Works, as well as how these safe-injection sites provide a safer environment for the community besides the drug users. Nina: What is the purpose of these safe injection sites? Shaun: The supervised injection services are designed to reduce public injection and discarded needles, and provide a safe and hygienic environment for people to come in and use the drugs that they’ve pre-obtained. So, it’s an overdose prevention service, meaning if someone overdoses here at the site or at the two that are coming, then we have nurses and other staff that can intervene, to support the person and give them naloxone or oxygen, to address their overdose. Nina: In terms of how the site works, do users have to sign in? Are they designated one nurse per person? How does the site work exactly? Shaun: Our site here at The Works is embedded in other services that we provide. People may come in to get harm reduction supplies, support, counselling, wound care, testing and vaccination. Also, the staff will let them know about the availability of the supervised injection service. Once they’ve identified that they want to use the service, there’s a really brief intake and assessment process next. The assessment covers points such as: What drugs are they using today? Have they overdosed before? Trying to assess what their overdose risk might be, following which they would go in and inject drugs under the supervision of the available staff. If they overdose then we can intervene to provide naloxone, oxygen or other measures. After their dosage they may move to the “chill out” or after injection space, where we can monitor them for about 15 minutes to ensure that they’re not experiencing an overdose. That’s also a place where we can provide some other services, so people generally might be more open to having a conversation about drug treatment, housing and support. Nina: And you’d mentioned earlier that the users come in with pre-obtained drugs. Therefore when it comes to drug laws, are there questions of where the pre-obtained drugs come from? Shaun: For the sites that have an exemption through Health Canada, people don’t have to fear arrest because of their drug use when they’re here. What happens outside, is beyond our control. But certainly, when they’re here, the staff and drug users are protected from the drug laws. Nina: Since opening the first interim site in August, and logging more than 800 visits, is there a limit on how many people can come to the site at a time and is there a time limit on how long users can stay? Shaun: The site was designed to accommodate as many people as we could, within the space that we have. We have five booths, and our hours when we’re up to full capacity will be 10am to 10pm, 7 days a week. We can accommodate five people at the injection booth, and probably five to six people in the after-injection space. We haven’t really had to rush people out because we’ve had the flexibility to have them here. But if it’s busy we probably would look at 15 minutes as the upper time limit in the after-injection area. Nina: In terms of rehabilitation services, is there anything that you offer or recommend users to head towards? Shaun: We do have a methadone program that operates out of here. It’s one of our existing services at The Works that we’ve had since 1998. So, if somebody wants to get on methadone or suboxone, we can talk to them about whether or not that program that we operate called Methadone Works, is the most appropriate place for them. And if not, we can refer them to another methadone/suboxone program in the community or to other drug treatment(s). We definitely would work with people on a good referral, and facilitating that referral for them, but it’s very self-directed. And if somebody expresses an interest in getting into treatment, that’s definitely something that we’ll work with them on. We’ll do everything we can to facilitate that referral, including potentially accompanying somebody to an assessment appointment. It can be (kind of) daunting to go to these appointments. We might be able to help with transportation, or we might even go along with them. But certainly, if somebody is using an opioid and would like to look at getting into our methadone program here, that’s an easy referral for us because it’s a service that we already provide. Nina: What do you say to people who are against the sites all together, in order to make them understand the bigger picture and the purpose that these sites serve to the community? Shaun: I think the supervised injection service meets the needs of both; the people who are using drugs and the community. This service, while preventing death from overdose and helping people to use better injection techniques, also identifies any wounds that they may need help with and provides counselling and support. Every injection that happens here, is an injection that doesn’t happen in the community. So, any supplies that people use; harm reduction supplies, needles, cookers - is not discarded in the community. It is discarded safely here. So I think this service is important, especially right now with all of the deaths caused by opioids in Toronto and across Canada and North America. This service can also meet the needs of the surrounding community. Nina: Since this is the first permanent safe injection site to open, do you see any loopholes or drawbacks in the structure? Shaun: You know, it’s a process to get this far. There’s an exemption application that you have to complete with Health Canada - and then getting funding and hiring staff. So, it’s a process. Even coming through as one of the first ones in Canada, I can say it’s been a long road, but it’s so worth it in terms of being able to offer this important service to our clients. Especially right now, with all of these concerns about overdose in the community.
It’s something that I think is very important. It provides a dignified place for people to use drugs. The people who have come through the service so far are really thankful and grateful that we’ve done this, so that they can feel safe and protected. I think there’s a lot of concerns in the community about overdose. People are scared and they’re just really grateful to be able to come in here and know that people are very non-judgemental, very supportive, and will intervene if they overdose. I’m proud to have been a part of this process and I think all of the staff here feel the same. |
Recent Posts
Categories
All
Archives
February 2022
|
|
GET THE APP!
Listen to VIBE 105 anywhere you go!
|
OUR STATION
|
TUNE IN RADIO
|
STAY CONNECTED
|
Copyright © 2021 Canadian Centre for Civic Media and Arts Development Inc. Except where otherwise noted, presentation of content on this site is protected by copyright law and redistribution without consent or written permission of the sponsor is strictly prohibited.






 RSS Feed
RSS Feed


